Reports From Dr. Catalona’s Follow-Up Studies | 2005
 Dr. Catalona and his research collaborators will be delivering their latest research findings at the American Urological Association (AUA) annual meeting.
Dr. Catalona and his research collaborators will be delivering their latest research findings at the American Urological Association (AUA) annual meeting.
Although the information is technical, the following summaries are written with QUEST readers in mind.
We would like to keep you updated on the direction of the research and the vocabulary associated with it.
Some of the information has practical applications now. Some shows the beginning of research projects with exploration or new understanding as the main purpose, and hopefully, practical applications will follow.
Surely, though, this research will define how prostate cancer is diagnosed, treated and hopefully prevented in generations to come.
PSA Correlates More Strongly With Percent of Cancer And Cancer Volume Than With Prostate Size
Although PSA testing is a widely used method of detecting early prostate cancer, a recent study argues that PSA is no longer a valid marker for prostate cancer but, rather, is only related to benign hyperplasia and prostate size. We had serious doubts about this study.
Question: Does PSA value correlate more strongly with percentage of cancer and cancer volume than with prostate size?
Using information from a radical retropubic prostatectomy (RRP) series of two groups, including 2273 patients treated from 1989 to 2001 and 926 patients treated from 2002 to 2005, we assessed the extent to which pre-operative PSA correlated with prostate weight, percentage of cancer, and cancer volume in the RRP specimen.
In both sample groups, prostate size was measured by the weight of the surgically removed prostate. Percentage of cancer was reported by patholiogists who examined sections from each case. Cancer volume was determined by multiplying the percentage of cancer by the prostate volume.
In both groups, correlation was consistently higher between PSA and percentage of cancer, and PSA and cancer volume, than between PSA and prostate size.
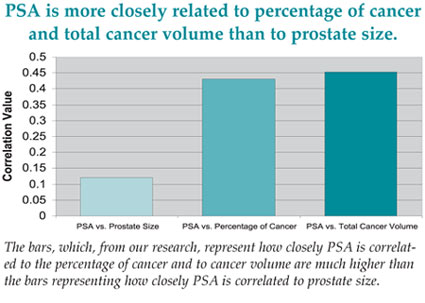
Only in patients with prostate volume larger than 55cc and with a tumor volume of less than 3cc does PSA correlate more strongly with prostate size. That group was only 11% of patients with complete data. The use of PSA density measurements (PSA divided by prostate volume) restored the significant correlation between PSA and percent cancer in the prostate.
Conclusion: PSA correlates with both prostate size and tumor volume.
The ratio of prostate volume to tumor size determines which correlation is stronger.
PSA correlates more strongly with tumor volume than with prostate size in most patients.
PSA density corrects for the effects of large prostate size in the remainder.
PSA is a valid marker for prostate cancer.
William J Catalona, Xiaoying Yu, Chicago, IL; Kimberly A Roehl, St. Louis, MO; Joannie T Yeh, Sara N Gashti, Chicago, IL; Jo Ann V Antenor, St. Louis, MO; Misop Han, Chicago, IL.
Recommending Biopsy Using PSA Velocity
The rate at which the PSA rises over a year is being used as a method for knowing when to recommend a biopsy.
Question: What PSA velocity should be the indicator for a prostate biopsy?
Previous studies have suggested that a PSA velocity (PSAV) of .75 ng/ml in a year is an appropriate cutoff for recommending a prostate biopsy, but few studies have been done using other PSAV cutoffs.
In a 10-year prostate cancer screening study, we looked at the results of PSAV and prostate cancer diagnosis in 26,000 men.
What we found is that a significant proportion of the men diagnosed with cancer (45%) had a PSAV of .5 ng/ml, and we found that the cancer detection rate using this cutoff is similar to the cancer detection rate at higher PSA velocity cutoffs.
Conclusion: Our results suggest that a PSAV of .5 ng/ml in a year should be a measure to recommend prostate biopsy.
Jo Ann V. Antenor, Kimberly A. Roehl, Saint Louis, MO; Misop Han, William J. Catalona, Chicago, IL

PSA Density and Prostate Cancer Aggressiveness
PSA density, which is the PSA value divided by the prostate volume, is an established measure for helping to determine the need for performing prostate biopsies, but data is limited on the association of PSA density with prostate cancer aggressiveness.
Question: Does PSA density have a connection with the aggressiveness of a prostate cancer?
The idea of using PSA density as a predictor of prostate cancer is that cancerous prostate tissue leaks more PSA into the blood than benign prostate tissue.
Thus, a man with a high PSA and a normal-sized prostate is more likely to have cancer than a man with the same PSA level and a large gland.
PSA in relation to the prostate size should reflect the volume of cancer in the gland.
We looked at the association of PSA density with features of tumor aggressiveness in patients who had localized prostate cancer treated by a radical prostatectomy.
What we found is that as PSA density increases, the trend for worsening pathology features of the cancer also increase.
Conclusion: PSA density measurements are useful as an aid to determining the aggressiveness of clinically localized prostate cancer.
Shilajit Kundu, Chicago, IL; Kimberly A. Roehl, St. Louis, MO; Xiaoying Yu, Chicago, IL; Jo Ann V. Antenor, St. Louis, MO; Joseph Pazona, Chicago, IL; Brian K. Suarez, St. Louis, MO; William J. Catalona, Chicago, IL
Pre-Treatment PSA Velocity:
A Possible Predictor for Success of Primary Radiation Therapy for CaP
PSA velocity (PSAV) during the year before diagnosis of prostate cancer has been shown to be a strong predictor of prostate cancer survival following treatment with radical prostatectomy.
Question: Does pre-diagnosis PSAV also identify men at increased risk for cancer progression after primary radiation therapy?
We identified 203 men with localized prostate cancer who were treated with radiation therapy from 1989 to 2001 and whose pre-diagnosis PSA information allowed us to calculate PSAV during the year prior to diagnosis of prostate cancer.
We studied the progression-free survival rate of these men after five years of follow-up.
Those men with a PSA velocity of less than 2 ng/ml had a progression-free survival rate of 80%.
Those men with a PSA velocity of more than 2 ng/ml had a progression-free survival rate of 62%.
Conclusion: PSAV during the year before diagnosis of prostate cancer is a predictor of cancer progression following primary radiation therapy.
Scott E Eggener, Chicago, IL; Kimberly A Roehl, Brian K Suarez, St. Louis, MO; William J Catalona, Chicago, IL






