Reports From Dr. Catalona’s Follow-up Studies | 2006
Age-Specific Risk of Prostate Cancer:
Intro: A man’s risk of developing prostate cancer increases if his baseline PSA is above the median for his age group. Many physicians 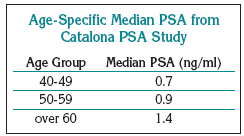 consider a PSA level of 2.5 or 4.0 ng/ml a threshold for prostate biopsy.
consider a PSA level of 2.5 or 4.0 ng/ml a threshold for prostate biopsy.
We looked at the risk of developing prostate cancer by age group when PSA lies between the median for the age group and these commonly used values.
?: Can PSA results be used more effectively if PSA is considered in conjunction with age?
Study: Between May 1991 and November 2001, we enrolled 26,000 men in a PSA and DRE-based screening study for prostate cancer. Men were put into groups by age and initial PSA and were screened at least annually.
Prostate biopsy was recommended if the PSA exceeded 4.0 ng/ml (before 1995) or 2.5 ng/ml (after 1995).
Men were put into 3 groups by age: ages 40 to 49, 50 to 59, and greater than 60 respectively. The median PSA was reported for each group. The relative risk of being diagnosed with prostate cancer was reported when PSA level was below the median value, between the median and commonly used thresholds for biopsy, or above 4.0 ng/ml.
The median PSA level was 0.7 ng/ml, 0.9 ng/ml, and 1.4 ng/ml for men in their 40s, 50s, and older than 60, respectively.
The risk of having prostate cancer detected was 0.2%, 0.7 %, and 2.7 % in the three groups, respectively, if the PSA level was below the median for his age group.
The relative risk of prostate cancer increased significantly as PSA increased above the median to 2.5 ng/ml or 2.6 to 4.0 ng/ml for each age group.
Although this effect was observed in all age groups, it was most pronounced in younger men. There was a trend towards higher positive margin rate and a lower rate of organ-confined disease with a PSA greater than the median for each age group. There was also a higher rate of PSA progression after radical prostatectomy if the PSA was above the median for the age group.
Conclusion: The risk of having prostate cancer increased significantly as PSA concentration increased above the median for each age group.
Younger men in particular were at significantly increased risk of developing prostate cancer, although these men were screened at an earlier age because they were deemed high risk due to factors like African-American race or family history of prostate cancer.
This information should be used to assess age-specific risk for cancer detection in PSA screening.
These men should be counseled about their risk of developing prostate cancer and they may benefit from more rigorous screening than their counterparts whose PSA level is below the median.
Baseline PSA screening at age 40 could be a significant help in determining a man’s subsequent risk for developing prostate cancer and detecting it at an early stage.
Shilajit D Kundu, Chicago, IL; Kimberly A Roehl, Jo Ann V Antenor, St. Louis, MO; William J Catalona, Robert B Nadler, Chicago, IL
PSA Velocity for Predicting Prostate Cancer in Young Men with a PSA of less than 4
Intro: Both prostate cancer and benign conditions of the prostate can cause a rise in PSA. PSA velocity is a way of distinguishing prostate cancer from benign conditions. A PSA velocity of 0.75 ng/ml per year has been the traditional marker for indications of cancer.
?: What does our data show regarding the PSA velocity threshold for distinguishing prostate cancer from a benign condition in young men with a PSA level less than 4?
Study: From 1989 to 2001, 36,000 men participated in a prostate cancer screen study. 6,844 were under 60 years old when the study began. 346 of these men were subsequently diagnosed with prostate cancer. In these men, PSAV thresholds were examined for prediction of prostate cancer risk.
Our data showed that a PSAV greater than 0.5 ng/ml per year was more predictive of prostate cancer than age, total PSA level, family history, or race. A study of a subgroup of these men whose PSA levels were less than 2.5 had similar results.
Conclusion: The traditional PSAV threshold for biopsy of 0.75 ng/ml per year is too high for men under age 60, and its use would result in missing a substantial proportion of prostate cancers.
Young men with a PSAV greater than 0.5 ng/ml per year are at a significantly greater risk for prostate cancer, and close follow-up is warranted.
Stacy Loeb, Washington, DC; Kimberly A Roehl, Saint Louis, MO; Theresa Graif, Davis Viprakasit, William J Catalona, Robert B Nadler, Chicago, IL
Long-Term Outcomes of Radical Prostatectomy for Clinically Advanced Prostate Cancer
Intro: Controversy exists regarding the preferred management of patients with clinically advanced prostate cancer.
?: What are the long-term cancer control and quality of life outcomes following radical prostatectomy in patients with borderline clinically advanced disease?
Study: We examined records of 288 men from 1984 to 2003 who had a Gleason score from 8 to 10 or a PSA level greater than 10 ng/ml. and who had undergone radical retropubic prostatectomy by a single surgeon. (William J. Catalona, MD)
We calculated the 7- and 10-year actuarial progression-free survival (PFS), overall survival (OS) and cancer-specific survival (CSS) rates. In addition we examined the rates of potency (excluding men who were not potent preoperatively) and continence.
At 7 years following surgery, the PFS, CSS and OS rates were 35%, 95% and 91%. At 10 years, the rates were 35%, 88% and 74%, respectively.
Conclusion: Overall, radical prostatectomy offers excellent cancer control at 10 years for some men of all ages presenting with borderline clinically advanced disease.
Potency and continence were preserved in the majority of patients, although the rates were significantly higher for younger men.
Radical prostatectomy with appropriate postoperative radiation and/or hormonal therapy is a reasonable treatment option for selected men with borderline locally advanced disease at time of detection.
Norm Smith, Chicago, IL; Kimberly A Roehl, Saint Louis, MO; Kelly Maxwell, Chicago, IL; Stacy Loeb, Washington, DC; Misop Han, William J. Catalona, Chicago, IL







